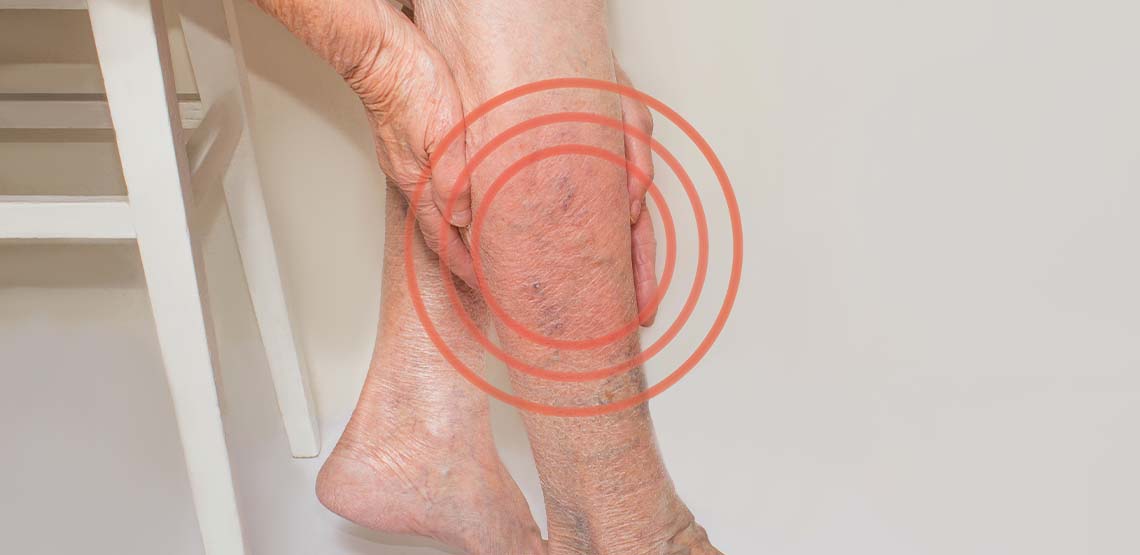
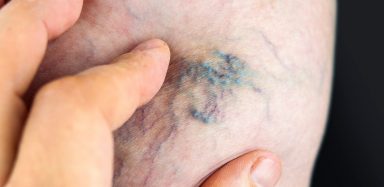
Varicose Eczema
Most people are familiar with the bluish enlarged veins commonly seen on legs and feet, called varicose veins. Though these veins may appear worrisome, varicose veins are not typically a health problem. However, in some cases, the skin surrounding the varicose veins may begin to itch and result in a condition called varicose eczema.
What is Varicose Eczema?
According to the National Eczema Society, about 70% of people who develop varicose eczema are over the age of 70. The skin condition, which is also known as stasis eczema or gravitational eczema appears as scaly, dry and flaky skin on the feet or lower legs. It develops due to high blood pressure in the surrounding veins, causing fluid to leak into the skin.
What Causes Varicose Eczema?
Because varicose veins are a sign of compromised circulation in the legs, the presence of varicose eczema is higher in people with varicose veins. Legs and feet are both farthest and lowest from the heart, and poor circulation causes blood to back up into the legs and feet.
To counter the effects of gravity and facilitate blood flow back to the heart, veins have valves to keep blood from flowing back down into the legs. These valves keep blood flowing one way and prevent blood from returning back down. In addition, the movement of muscles surrounding the veins helps with blood circulation.
Unfortunately, increased blood pressure causes the small valves in the leg veins to stop working correctly, which allows fluid to leak into the surrounding tissue. This leaked tissue causes the body’s immune system to react, resulting in varicose eczema symptoms.
The following factors may place a person at a higher risk for developing varicose eczema:
- Being female.
- Being pregnant, as it increases pressure within the legs.
- Living a sedentary lifestyle, as immobility affects circulation and can damage valves in the veins.
- Being an older adult, as you might have higher rates of circulation problems, leading to varicose eczema.
- Obesity, as it can raise the pressure within the veins, especially within the legs.
What Are the Signs and Symptoms of Varicose Eczema?
The signs and symptoms are much like those of chronic eczema. The symptoms may come and go, with periods of varying severity. When affected, the skin becomes:
- Swollen.
- Itchy.
- Crusty.
- Scaly.
- Flaky.
- Dry.
Light skin may develop red or brown areas. On darker skin, the areas can look purple, gray, or dark brown. In these areas, enlarged, swollen varicose veins are present.
Top 5 Treatments for Varicose Eczema
A multifaceted approach is typically the best way to treat varicose eczema.
1. Soak and Seal
The National Eczema Association recommends an at-home soak and seal approach to reduce the symptoms. This process involves soaking the affected area in lukewarm water for 10 minutes, then patting the area dry until damp. Soon after, at least within three minutes, apply moisturizer to the area to seal in water. If a topical medication is prescribed by a healthcare provider, use it prior to the moisturizer, as it can help alleviate symptoms.
2. Topical Corticosteroids
A corticosteroid doesn’t have to be powerful to address eczema symptoms. Even a low-potency or moderate-potency corticosteroid can offer satisfactory results. A published review of 30 different topical steroids found that not only are low-potency and moderate-potency steroids effective, but they also have fewer side effects than stronger potencies. Most topical steroids require a doctor’s prescription, but low-dose steroids are available over-the-counter and work against many types of eczema.
Related Search Topics (Ads)
3. Compression Stockings
Rather than treating the eczema itself, compression stockings target the cause — varicose veins. Compression stockings are specially designed socks or stockings that squeeze the lower parts of the leg and loosen the further up they go. When getting compression stockings, consult your healthcare provider to find the right size. These stockings are worn every day and help reduce blood pooling in the legs.
4. Moisturizers
Applying moisturizer directly onto the skin can help to minimize redness and repair the skin barrier, which eczema can destroy. Moisturizers soothe damaged and flaky skin. They also keep water locked into the skin, which hydrates dry areas and reduces itching. When choosing a moisturizer, look for one that’s free of harsh fragrances, and remember to use the soak and seal approach.
5. Elevate Your Legs
Lifting your legs above your heart during sleep can boost blood flow and prevent blood from pooling in the legs. A pillow or two under the legs at night can counter the effects of gravity and keep blood circulating to the heart. Furthermore, walking, exercising and elevating the legs throughout the day can also boost blood flow and keep blood from pooling.
When to Seek Medical Attention for Varicose Eczema
Varicose veins and eczema are treatable, so it is essential to see your healthcare provider for either condition. However, if you have tried at-home treatments or notice any significant discoloration, heat, pain, or excessive swelling, see your healthcare provider right away.
Getting Treatment for Varicose Eczema
Although it isn’t life-threatening, the itching and swelling can become bothersome. Furthermore, some individuals may consider their varicose veins and varicose eczema unsightly and seek out treatment. If varicose veins and eczema are affecting your life, consult with your healthcare provider to talk about your treatment options.