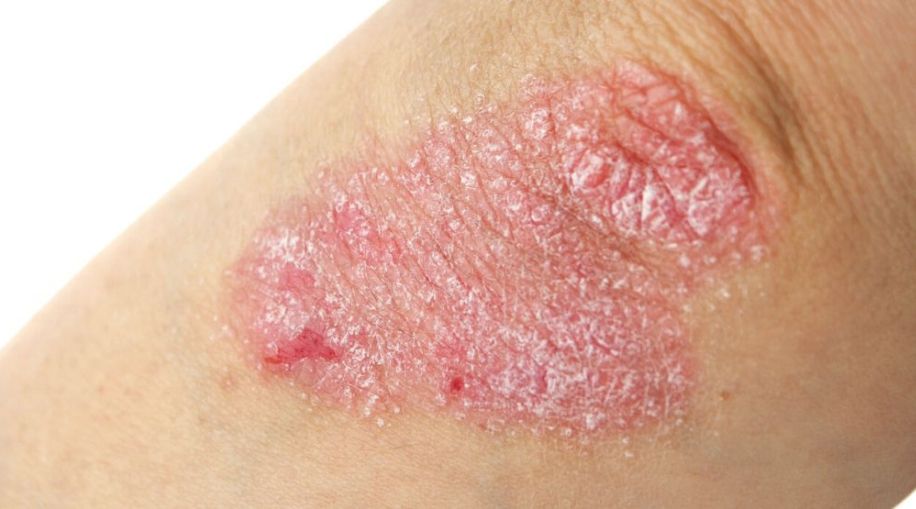
What is Psoriasis and How is it Treated?
Psoriasis is a common chronic, inflammatory disease with skin and joint involvement. While it manifests primarily as a skin disorder, characterized by red, scaly, itchy and thickened patches, it is also associated with many medical and psychiatric conditions, including psoriatic arthritis, heart problems, diabetes, anxiety and depression. A common medication used for treatment is Otezla. Otezla is a medication used to treat autoimmune disorders, such as plaque psoriasis and psoriatic arthritis. It helps stop inflammation and can be used to reduce discomfort associated with joint pain, swelling and stiffness.
10 Psoriasis Triggers
- Stress.
- Cold and Dry Weather.
- Infections.
- Certain Medications.
- Skin Injuries.
- Smoking.
- Heavy Alcohol Consumption.
- Hormonal Changes.
- Obesity.
- Genetics.
Symptoms of Psoriasis
There are many symptoms of psoriasis to look for. These are ten common psoriasis symptoms to be aware of:
- Red, inflamed patches on your skin.
- Itchy or painful skin.
- Dry, flaky, or scaly-looking skin on your scalp (similar to dandruff).
- Discoloration, dents or other abnormal changes to your nails.
- Joint or pain stiffness.
- Drop-shaped lesions on your skin.
- Patches of skin that look silver or white, and are flaky.
- Issues sleeping.
- Rashes that flare up for weeks at a time and then go away.
- Bleeding in areas where the skin is itchy.
Psoriasis Classification
Psoriasis lesions can present anywhere on the body but are usually found on the trunk, scalp, elbows, limbs, knees and body folds. Clinicians classify the severity of the disease as mild, moderate, or severe based on the following parameters.
Mild Psoriasis
- Less than 5% of the body surface area (BSA) is involved.
- The disease does not alter the patient’s quality of life.
- It responds to treatments with no known serious risks, or may not require any treatment at all.
Moderate Psoriasis
- Between 2% to 20% of BSA is involved with the disease.
- Therapy will improve the patient’s quality of life.
- Treatments used may have minimal risks.
Severe Psoriasis
- More than 10% of BSA is involved with the disease.
- Does not respond to treatment with minimal risks.
- The disease alters the patient’s quality of life.
Related Search Topics (Ads)
Types of Psoriasis
Psoriasis has an unpredictable and variable clinical course; you may experience periods of high and low disease activity. The most common presentation of the disease is widespread, well-demarcated, reddish, scaly plaque that may be itchy or painful. The color of the lesion varies, depending on skin type and localization.
The acute forms may have a bright reddish color. In some cases, the reddish plaques are covered by silvery scales seen frequently on the elbows, knees, and lower back. Psoriasis is further categorized based on its clinical characteristics: the appearance of the lesions and where they are localized. Below are the most common varieties.
Plaque
Plaque-type psoriasis, also known as psoriasis vulgaris, is the most common type of psoriasis. It accounts for over 80% of all cases. It is also the most extensively studied form in clinical trials. The red, scaly, thickened lesions are often large and appear on elbows, trunks, knees and legs.
Guttate
Less than 20% of patients suffer from this form of psoriasis. Guttate lesions are small, red papules that can be found all over the body, and commonly affects children and young adults. Characteristically, the sudden appearance of multiple papules is preceded by a streptococcal sore throat. New lesions may continue to appear within two to three months, and then resolve spontaneously.
Pustular
Generalized pustular psoriasis appears as multiple tender pustules (blisters) on a blotchy, reddish base. This rare form affects less than 2% of patients. It is often seen as a flare after a triggering event, such as stress, medications, infection or certain chemicals.
Erythrodermic
Erythrodermic is a rare variant of psoriasis with a whole-body presentation. Like pustular psoriasis, attacks or flare-ups can develop as a reaction to certain medications, stressful events, sunburns and withdrawal of oral steroids. This type is considered a severe condition and may require hospitalization and systemic therapy.
Subtypes According to Anatomical Location
Now that you know about the main types of this health condition, it is also good to learn about the subtypes. Here are what the subtypes include.
Palmoplantar Psoriasis
The lesions are localized to the hands and soles of the feet. They may appear as scaly and thickened patches or pustules, or both. The thick skin of the palms and soles affects the penetration of topical medications.
Inverse Psoriasis
Inverse or flexural psoriasis can be seen on the groin (or “jock itch” area) in men and on skin folds under breasts in women. The skin folds are sensitive to the side effects of steroids, which can be hard to treat.
Nail Psoriasis
Psoriasis that affects the nails imparts additional symptoms such as nail pitting and loosening or separation of the nail from the nail bed (onycholysis). Current treatments available for this condition are limited and have poor response.
Scalp Psoriasis
In this type, the lesion can affect the whole scalp; sometimes the lesions are more localized. Hair growth may be impaired, causing cicatricial alopecia or hair loss.
Causes and Risk Factors
The exact cause of psoriasis is still unclear. It is believed that genetics, environmental factors and immunological mechanisms play a role. Most complex diseases have no single cause, but a range of interacting risk factors.
Certain environmental triggers are said to disrupt the integrity of the skin immune system in individuals with a genetic predisposition to psoriasis. Medications that may induce or make psoriasis worse include angiotensin-converting enzyme inhibitors (blood pressure drugs), antimalarials, lithium and nonsteroidal anti-inflammatory drugs. Infections and trauma (Koebner phenomenon) to the skin can also trigger a flare-up.
Treatment Options
Topical treatments can provide relief as well as safety in patients with mild to moderate disease. Those with moderate to severe psoriasis may use short-term topical treatments as part of a combination regimen to minimize doses of systemic drugs and phototherapy.
Topical Treatments
In the U.S., topical corticosteroids are the mainstay of therapy. Three out of four psoriasis patients are treated with topical corticosteroids. They come in different formulations (ointments, lotions, creams, sprays) and have a high safety profile than other types of therapies. Other topical medications used for psoriasis are Vitamin D analogs, retinoids, salicylic acid, calcineurin inhibitors, emollients and coal tar.
Oral Medications
Methotrexate (MTX) was officially approved by the FDA in 1972 for use in patients with severe, disabling psoriasis. It can be used in combination with other oral agents, topicals and phototherapy. Other immunosuppressant drugs for psoriasis include cyclosporine and mycophenolate mofetil.
Phototherapy
Phototherapy or light therapy uses specialized lights to deliver UV radiation onto a patient’s skin. This is the next therapeutic recommendation for moderate to severe psoriasis following topical treatments before initiating oral or systemic therapies. The application of corticosteroids after each session can be used to avoid worsening the redness and inflammation.
Biologic Therapies
The safety profile of biologics is still under study. These protein-based drugs were developed to modify the immune system response by targeting the immune cells that cause psoriasis. They are given by injection or intravenous infusion. TNF alpha inhibitors (etanercept, adalimumab, infliximab); interleukin 12 and 23 inhibitors (ustekinumab); and T-cell inhibitors (abatacept) are some of the biologics approved for psoriatic disease.
Preventing Flare-ups
Psoriasis with triggers can easily be prevented by avoiding the cause of flare-ups. Lifestyle factors such as alcohol consumption, smoking and obesity may affect the severity of the disease. Alcohol stimulates the release of histamine, which makes the skin itchy and prone to lesions.
Physical activities and exercise are known to be beneficial. Stress management, in the form of yoga and meditation, can also be beneficial. Milk and gluten can exacerbate symptoms in some people, while food high in anti-inflammatory omega-3 fatty acids is recommended.
Sun exposure is helpful because it increases Vitamin D levels in the body but getting sunburned can increase the risk of skin cancer.
Treatment for should be individualized so it is important to consult a dermatologist to get proper treatment and symptom management.
Although psoriasis is not a life-threatening condition for most people, it significantly impacts a person’s quality of life. The World Happiness Report 2017 revealed that psoriasis greatly reduces a person’s happiness level by 30%. Thus, the goal of treatment is geared toward minimizing skin changes and improving quality of life.